|
OTHER MINOR PROCEDURES AND OTHER NEURALGIAS
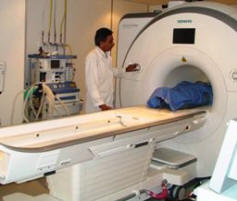
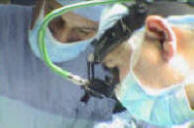
 Microvascular Decompression;
Abnormalities at the Trigeminal Nerve Root Entry Zone
Microvascular Decompression;
Abnormalities at the Trigeminal Nerve Root Entry Zone
A steadily
increasing number of neurosurgeons are so favorably impressed with the
results of microvascular decompression (MVD) of the trigeminal root
entry zone at the pons in the treatment of trigeminal neuralgia that
they recommend this for all but medically infirm or older patients when
medical management becomes unsatisfactory. The principal uncertainty in
the minds of some of us is the extent of the pressure on the trigeminal
rootlets required to provoke the syndrome. In some
cases causative pressure by one or more arteries exists. Jannetta described
"neurovascular compression" at the root entry zone in 395 (96 percent)
of 411 patients with trigeminal neuralgia. Zorman and Wilson stated that "veins and arterial loops not in direct
contact with the root were presumed to be causative if they were in
close proximity to an anatomically deformed nerve root because
retracting the cerebellum could displace the pons and trigeminal root
away from an offending artery or vein. They found causative
extrinsic lesions in 79 percent of 125 patients. Their results after MVD
were about the same whether they treated presumed venous or arterial
compression or, finding neither, did a partial sensory rhizotomy (PSR).
Breeze and Ignelzi likewise considered the finding of a vessel "near"
the nerve in 37 percent of their 52 procedures as indicative of the
cause of the pain.
In a 1989 review of 252 patients with
trigeminal neuralgia treated between 1969 and 1985, Wilson's statements
seem to reflect a striking change in his criteria for determining
treatment of significant compression of nerve by blood vessel. When the
nerve root is "distorted" by an artery and/or a vein, he does an MVD by
coagulating and dividing veins, and by dissecting arterial loops from
the nerve root. This displacement is maintained by a small sculpted
prosthesis of sponge Teflon inserted between the root and the vessel.
One drop of cyanoacrylate cement is used to secure the prosthesis to the
pia or nerve root. Patients in whom vascular contact was found
without deformity of the nerve root underwent both displacement of the
vessel (MVD) and PSR consisting of section of the inferior one-half to
two-thirds of the portio major. Patients in whom no vascular contact was
found underwent PSR only. Using these criteria he performed MVD only in
166 (66 percent) of the cases, MVD and PSR in 56 (22 percent), and PSR
only in 30 (12 percent). Seven local tumors and two arteriovenous
malformations (AVMs) were included in the group undergoing MVD and no
PSR. In 1984, Wilson published a review of 118 of the earliest cases of
this series and reported that 92 (78 percent) underwent MVD only while
26 (22 percent) had a PSR; none had both procedures. In this earlier
series the therapeutic results in the two groups were indistinguishable.
In the same year, however, Piatt and Wilkins described a drop in the
success rate of MVD from 83 percent to 62 percent when the artery and
nerve were merely in contact. Wilson was apparently impressed by this
observation, because in his later publication he added PSR to MVD in
the management of this arterial contact group. The resultant percentages
in the "excellent" and "good" categories were slightly better in these patients than in
those who had only one of the two procedures. In these latter two groups
the outcomes were about the same. With respect to
complications, Wilson achieved a major triumph, with no deaths and no
lasting deficit of any significant function in any patient. In seeking
to match his surgical judgment and dexterity by his mental agility,
Wilson argued that posterior fossa exploration should be the firstline
therapy, stating that even successful prolonged "medical treatment may
ultimately reduce the efficacy of surgery." He and Alksne have drawn
attention to their finding that any proximal ablative procedure,
including any percutaneous tactic in the middle cranial fossa, decreases
the likelihood of success of a subsequent MVD. But, as Jannetta (1985)
asks, "are these patients just less amenable to any therapy?" It is
obvious that ease of controlling the paroxysms of trigeminal neuralgia
varies enormously from case to case. In Wilson's series a second
posterior fossa procedure was performed in 20 patients with persistent
or recurrent pain. In no patient had the prosthesis shifted so it was
left in place. He logically did a PSR in 18 of the 20 patients, 7 of
whom had undergone a PSR at the first operation, achieving an excellent
or good result in 85 percent. It seem that Wilson had general shift to
requiring more reasons for doing a PSR that he is less confident
that extrinsic vascular compression causes most of the cases of
"essential" trigeminal neuralgia.
Wilson also pointed out that his'
'excellent" results were in patients who had a shorter duration of
symptoms (average 7.4 years) than those in the "good," "recurrent," and
"poor" categories; accordingly, in his view we should operate
early "before the nerve is irreversibly damaged." However, his "good"
category's average duration of symptoms of 10.5 years is much longer
than the worse "recurrent" and "poor" categories. This argument for
early operation is made the flimsier by his finding that the younger the
patient at the onset of the symptoms, the worse the result of MVD. Hence
in those 20 who failed to maintain benefit from sustained adequate
decompression as well as in the 30 who never had any evidence of
extrinsic compression, totalling 20 percent of the 252 cases, such
compression did not cause their pain.
The French neurosurgeon Sindou and his
colleagues are the only ones who have compared the cerebellopontine (CP)
angle findings at operation between patients with trigeminal neuralgia
and those with facial pain due to neoplasm. Among 150 patients in the
former group they found a vasculoneural "conflit" in 132 (88 percent) of them. A further 14 patients (9 percent)
had some other obvious lesion. However, they found a vasculoneural "conflit"
in not a single one of 52 patients in whom they were doing a trigeminal
rhizotomy for pain due to tumor located away from the sensory root.
Sindou and colleagues have thoughtfully
attempted to determine whether the pain-relieving feature of
"microvascular decompression" is really the removal of a compressive
lesion-the vein or pulsating artery- or is merely another form of
compression-a "neocompression." Does an interposed substance-muscle
or other material-between the nerve and vessel simply shift from a
vascular to another form of constant compression of the rootlets,
analogous to the temporary frank rootlet compression of the open or
percutaneous operations in the middle cranial fossa. Accordingly they
studied decompression by two relevant differing methods. In two
clinically similar groups, each of 60 patients with trigeminal
neuralgia, the first group had the artery dissected away from the nerve
and maintained in that position by the interposition of foreign material
(Dacron) and at times some periosteum as well between the artery and
nerve. In the second group the offending vessels were dislodged without any
material touching the nerve. The artery was held away from the nerve by
Teflon strips, at times with a 7 x 10 mm piece of Dacron also. A
follow-up at 1 year revealed a recurrence rate of 10 percent in the
first group and 4.5 percent in the second. They concluded that a "true
decompression" rather than a "neocompression" was the more effective
type of operation.
Electron microscopic study of the
rootlets distorted by the blood vessel and of other specimens maximally
removed from the site surely is the most direct way to secure relevant
data as to the cause of the paroxysms.
At the other end of the scale are the
observations of Adams et al., who saw "Indentation, grooving, or
distortion of the nerve by a vascular structure" in only 6 of 57
patients explored in the posterior fossa. Similarly Rovit noted such
finds in only 2 of 25 patients.
Postmortem studies to determine the
neurovascular relationships in patients without facial pain are about
as divergent as the in vivo observations on those with trigeminal
neuralgia. The four publications to evaluate are those of Hardy and Rhoton (1978), Haines et al. (1980), Mehta et al. (1981), and Klun
and Prestor (1986 ). The first group saw arterial contacts in 52
percent of 50 CP angles, "often" with arterial compression. In
contrast were the observations of Mehta et al., who saw arterial
contacts with the trigeminal root in only 13 percent of 60 CP angles,
and no distortion of nerve by artery. The following were the figures
in non-tic cadavers of Haines et al. in 40 CP angles: 25 percent
arterial contact, 23 percent venous contact, and 10 percent
compression. The corresponding figures of Klun and Prestor in 130 CP
angles were 23 percent, 4 percent, and 7 percent.
In view of the far higher percentages in
the cadavers of contacts, arterial or venous, than of
compression recorded by all four groups, it clearly makes sense to
correlate the percentages achieving pain relief with the various types
of neurovascular relationship. The first ones to do this. Piatt and
Wilkins, found that when an artery distorted the root or was wedged
between the root and the pons, as seen in 37 cases, MVD realized an
expected cure rate of 83 percent. This dropped to 62 percent of 31
cases when the artery to rootlet relation was one only of contact. A
further drop to 42 percent occurred in those with merely venous contact
or distortion, or "no abnormality." Their highest percentage of
excellent and good results ensued in their 21
patients in this last status on whom they did a PSR.
 Comparison of Results of Minimally Destructive Operations in the
Middle or Posterior Fossa
Comparison of Results of Minimally Destructive Operations in the
Middle or Posterior Fossa
There is good evidence that there is
some other causative factor in the
majority of cases not related to the anatomy of the root entry zone at
the pons or the nearby root beyond that zone. These begin with the
results of the various largely nondestructive operations in the middle
cranial fossa carried out in the fifties and sixties in an effort to
avoid the deafferentation dysesthesia (anesthesia dolorosa) of
trigeminal root section. A variety of procedures were performed. Taarnhoj stayed with his
proposal of "decompression" by incising the length of the dural
roof of the trigeminal cistern. Shelden et al. noted that their original
concept of "decompressing" the peripheral second and third divisions at
the foramina rotundum and ovale gave about the same results as the
Taarnhoj operation. They decided that the feature common to the two
manoeuvres was probably modest trauma to the trigeminal pathways; hence,
they changed the decompression to "compression," rubbing vigorously the
ganglion and rootlets with a blunt instrument after opening the dura
over them. Several minor variations on these concepts were proposed by
other neurosurgeons. Thus Gardner "frees the sensory rootlets from their
dural sleeve, gently touches them with a cotton pledget, and sprays them
forcefully with a Ringer's solution." Other modifications of local
manipulation by six other neurosurgeons (summarized by White and Sweet)
all shared the feature of cutting no rootlets. Over 1600 cases thus
treated had been reported by 1969.
|
TABLE-1 Results of Minor Manipulations in
the Middle Fossa |
|
Reference |
Number of Patients |
Initial Failure+ Significant Recurrence (%) |
Duration of Follow-up
(Years) |
|
Bohm & Hojeberg |
111 |
24 |
22% |
2-4 |
|
Gardner & Miklos |
102 |
25 |
25% |
3.5-5.5 |
|
Graf |
100 |
26 |
26% |
Up to 8 |
|
Hamby |
88 |
7 |
8% |
Up to 6 |
|
Rowe |
96 |
14 |
15% |
|
|
Shelden |
200 |
50 |
25% |
Up to 10 |
|
Taarnhoj |
230 |
93 |
40% |
Up to 20 |
| |
|
|
|
Avg >12 |
|
Totals |
927 |
239 |
26% |
|
Several
reports describe the great majority of recurrences as taking place
within the first year or two both for the middle fossa manipulations
and for MVD in the posterior fossa. Although after both types of
operation there may be a period of some days to a week before the
neuralgic pains subside, they did so after the middle fossa procedures
in all but 3.8% reported by 14 surgeons. After MVD, initial sustained failure occurred in 6.7% in
eight reports.
Dahle et al. in their 57 cases found that
the procedures failed to give complete relief in 44 percent of their
patients (average followup only 3.1 years. Their results included
one fatal cardiac infarction at 1 week; recoveries from a hemiparesis
and partial bulbar palsy at 3 months, and from bacterial meningitis in
two cases; and two permanent sequelae- a patient with severe hemifacial
sensory loss and another with unilateral deafness and disabling
dysesthesia. That these surgeons should continue with MVD operations in
the face of the data on percutaneous operations is interesting.
 Results of Retrogasserian
Glycerol Injections
Results of Retrogasserian
Glycerol Injections
The procedure, pioneered by
Häkanson, of injecting glycerol into the fluid of the tiny
trigeminal cistern has found favour in many quarters because
of the minimal numbers of patients developing dysesthesias
and showing any lasting significant trigeminal sensory loss
after such injections. Once the small quantities of
glycerol injected leave the cistern they are diluted by the
much larger volumes of CSF in the CP and cerebellomedullary
cisterns. Hence, this toxic effect must be confined to that
portion of the rootlets in the middle cranial fossa. Several
authorities consider glycerol as their first choice when the medical
management of trigeminal neuralgia has failed. Although the
percentages of early and late failures exceed those of
either of the two open operations discussed, the modest
degree of sensory loss may be comparable. There is
essentially no mechanical manipulation of the rootlets
involved and this may account for the less favourable
results. As with the other procedures, the longer the
follow-up the higher the recurrence rate. De la Porte et al.
state only that the rate of pain relief was lower than that
with thermocoagulation or percutaneous compression.
A point to be noted, the
tendency of the glycerol to strike V1 fibers more often than
those in the second and third divisions, has been much more
quantitatively shown by Bergenheim, Hariz, and Laitinen.
They measured the thresholds for facial pain perception in
milliamperes at six standard sites (using the ISSAL 1412
apparatus), delivering a constant current to bipolar
electrodes. The day after the glycerol instillation into the
trigeminal cistern in 57 patients the threshold current for
perception of any sensation and the higher threshold for
pain were increased as compared with preoperative
thresholds. They say this increase "was especially marked
and well localized for those with pain in the first branch."
(This loss need not extend to corneal anesthesia.) The
absence of any sensory loss and minor sensory loss in the
remainder characterized the first 100 patients of Häkanson
and preservation of much or all
sensation was the finding of most, but not all, of the 22 rapporteurs. There is essentially no mechanical manipulation
of the rootlets or increased pressure against them and this
may account for the less favourable results. As with the
other procedures, the longer the follow-up the higher the
recurrence rate. However, the fact that the majority have
long-lasting relief associated with minimal sensory loss
adds another large group of patients to those whose relief
cannot be attributed to any change in neurovascular
relations at the trigeminal root entry zone into the pons.
 Conclusion upon Comparison
of Open Operations
Conclusion upon Comparison
of Open Operations
The similarity between the
general results in the two groups of open operations is
striking. The likelihood of modification by middle fossa
manipulations of anatomic relationships at the pontine
trigeminal root entry zone is so small that the hypothesis
that local pressure there causes the pain
is for the great majority of cases untenable by virtue of
this set of facts alone. Adams, in a commendable detailed
analysis of many factors bearing on the hypothesis, has
adduced an impressive array of considerations leading to the
same conclusion, none of which alone seems as telling
a refutation of the hypothesis as the results of minimally
destructive middle fossa operations. However, taken in toto
they add up to a major challenge to, but do not disprove,
the concept of vascular compression as the most common cause
of trigeminal neuralgia. Scepticism as to the validity of
this concept comes as a bitter disappointment to many
neurosurgeons. The microneurosurgery involved
in "vascular decompression" is such a delightful exercise
that it saddens to recommend great reduction in its usage
because its mortality and morbidity cannot be reduced to the
levels of the percutaneous operations.
 Other Evidence of the Salutary Effect of Manipulation Near
the Nerve
Other Evidence of the Salutary Effect of Manipulation Near
the Nerve
Parkinson recently described a
60-year-old patient at whose middle fossa operation in 1940
he assisted another neurosurgeon. The trigeminal nerve was
never identified in the 4-h operation, at which much packing
and coagulating occurred. Sensation in the face remained'
'perfect." The patient never suffered any more trigeminal
pain for the 35 years of follow-up.
Other modest manoeuvres near
the trigeminal pathway may stop the severe
paroxysms-mysterious though this mechanism may be.
 Relief after Minor
Extracranial Manipulation
Relief after Minor
Extracranial Manipulation
Entering an
artery subcranially (presumably the internal carotid artery)
instead of the foramen ovale and stopping the procedure,
which could possibly lead to
a small embolus breaking off from the puncture site within
the lumen and causing occlusion of a significant
intracerebral artery. Such subcranial arterial puncture
occurred in several patients. Remissions from 1 month to over a
year occurred in 60% of them. The prompt appearance of a
large hematoma on the cheek had led
to stopping the procedure before entry into the foramen
ovale, led to permanent recovery from the neuralgia in
several reports.
 Relief after Minimal
Intracranial Manipulation
Relief after Minimal
Intracranial Manipulation
Relief after such procedures
has occurred in three of Sweet W.H. cases. He reports the
following:
1. A 45-year-old man with
second-division trigeminal neuralgia for 4 years. In February 1967,
a pair of electrodes in a plastic cuff was slipped easily
around the second division of the trigeminal nerve just
behind the foramen rotundum. The objective was to test the
efficacy of chronic electrical stimulation of the trigger
zones that were confined to this division. He was not
stimulated at operation, but awoke pain-free and remained so
for 8 years before recurrence developed at the same site.
(This pain was then not altered by electrical stimulation.)
2. A 48-year-old man who had
had third-division trigeminal neuralgia for 6 years, during
which there had been no drug-free remission. An atypical
feature was hypalgesia of the second and third trigeminal, vagoglossopharyngeal, and upper cervical nerve zones.
Although this cleared after a normal pneumoencephalogram, I
elected to expose the CP angle. In August 1975, an unusually
easy exposure of the fourth and fifth nerve rootlets aided
by the absence of any obscuring veins permitted minimal
cerebellar retraction to disclose the single large straight
superior cerebellar artery nearer the fourth than the
fifth rootlets. No instrument or cottonoid was ever less
than a centimetre from the trigeminal rootlets. The rootlets
IV through XI and their relations to vessels were also
normal. The wound was closed with the intention of making a
radiofrequency lesion. This was never needed, because the
patient remained pain-free until death from a myocardial
infarction 10 years later.
3. A 77-year-old woman with
typical first- and second-division trigeminal neuralgia for
20 years had had her longest remission 2 years earlier for
about 2 months. Placement of a 20-gauge electrode through
the foramen ovale to a point 8 mm behind the dorsum sellae
and 5 mm above the horizontal plane of the sellar floor was
obviously above the trigeminal rootlets as shown also by
failure of electrical stimulation to evoke a response.
Inasmuch as the cerebrospinal fluid from the needle
electrode continued somewhat bloody after 13 ml, the
procedure was terminated. There was no trigeminal sensory
loss, or other sequel, but complete pain relief persisted
for 5.5 months. On one other occasion in which I
terminated a procedure without a lesion because of
intracranial arterial bleeding, there were no sequelae but
no relief of pain.
Varma and Frazer observed
vascular "contacts" with the nerve in the CP angle in 13 of
20 patients with trigeminal neuralgia. Of the 7 without
such contact, 3 had multiple sclerosis. They wrapped the trigeminal nerve with
muscle in 19 of the patients. Only in a 20th patient with
multiple sclerosis did they cut the nerve, with complete
relief. All 19, except the 2 with multiple sclerosis, were
also completely relieved during follow-ups from 4 to 30
months.
Nugent and Rovit seek to stop their lesions upon
achieving "minimal hypalgesia or analgesia" in the trigger
zones. Their recurrence rates are about the same as those
of the rest groups. Hypalgesia is much less likely to be
accompanied by dysesthesias, and attainment of this level of
sensory loss may well suffice for many of the patients.
|